Multidisciplinary Management of Clcp
M3 India Newsdesk Jan 07, 2025
This article explains the embryology, types, causes, epidemiology and management of the Cleft lip and palate (Clcp) or CLP. It also talks about the challenges and associated anomalies of this condition.
- The most prevalent birth abnormality affecting the head and neck is an orofacial cleft.
- 50% of orofacial clefts are of palate and lip (CLP).
- It is characterised by speech, hearing, middle ear abnormalities and dental psychosocial issues.
Embryology
- First trimester- Critical for lip and palate development.
- 4th week IU- Facial prominences.
- 5th week- Palate formation begins.
- 7th week- Fusion of medial nasal prominences; primary and secondary palate formation.
- 8th -12th weeks- Fusion of palatine shelves (incisive foramen to uvula).
Cleft lip
- Failed merging of the maxillary and medial nasal elevations.
- One or both sides.
- Inadequate migration of neural crest cells.
Cleft palate
- The lateral palatine processes' inability to meet and join.
- Defective growth of the palatal shelves.
- Failure of the shelves to rise above the tongue.
Types of cleft lip and palate
1. Based on the extent of the cleft
- Complete cleft
- Complete cleft lip involves the entire vertical thickness of the lip; associated with cleft of the alveolus.
- Complete cleft palate involves both primary and secondary palates and alveolus.
- Incomplete cleft
- The incomplete cleft of the lip has a band of tissue intact across the cleft.
- Isolated cleft palate involves the secondary palate, posterior to the incisive foramen.
2. Based on the side affected
- Unilateral cleft
- Bilateral cleft
3. Genetic classification
- Syndromic
- Non-syndromic
Causes
- Isolated mutations (syndromic/non-syndromic)
- Environmental factors
- Teratogen exposure (alcohol, tobacco)
- Combination
Syndromic CLP
- Associated congenital defects:
- Cardiac malformations
- Intellectual disabilities
- 30% CLP and 50% cleft palate cases
- Teratogens, chromosomal alterations or genetic mutations
- Van der Woude syndrome
- Velocardiofacial syndrome (DiGeorge Syndrome)
- CHARGE syndrome
- Beckwith-Wiedemann syndrome
- Apert syndrome
- Pierre Robin Syndrome
- Treacher-Collins Syndrome
- Klippel Feil Syndrome
- Goldenhar syndrome
- Stickler syndrome
Epidemiology
- Overall incidence- 1.5 (220,000 cases per year)
- Isolated CL- 25% of all clefts
- Combined CLP- 45% of all clefts
- Unilateral: Bilateral clefts- 4:1
- 70% unilateral clefts- left side of the face
- CP- more common in females
- 40%of all clefts- familial tendency
India
- CLP- 9.3 per 10,000 live births (22,786 infants each year)
- CP- 1.7 per 10,000 live births (4,145 infants each year)
Challenges and associated anomalies
- Micrognathia | Glossoptosis | CLP – Pierre-Robin Sequence
- Airway obstruction (tongue malposition)
- Difficulty in feeding (inability to create suction)
- Otitis media and other middle ear anomalies
- Dental anomalies
- Tooth rotations
- Enamel hypoplasia
- Missing Teeth
- Supernumerary teeth
- Hypodontia on the cleft side (lateral incisors)
- Dental caries (more in maxilla)
The cleft lip and palate team



Sequence of treatment
- Stage I- Infant Appliance Stage: Birth To 18 Months of Age
- Stage II- Primary Dentition Stage: 18 Months To 5 Years Of Age
- Stage III- Late Primary Or Early Mixed Dentition Stage: 6 To 10 Or 11 Years Of Age
- Stage IV- Permanent Dentition Stage: 12 To 18 Years Of Age
1. Stage I- Infant appliance stage: Birth To 18 months of age
Newborn: feeding problems addressed by the Nurse
- Insufficient suction to pull milk from the nipple
- Excessive air intake during feeding (requiring several burpings)
- Choking
- Nasal discharge
- Excessive time required to take nourishment
The maxillary obturator
- Provides false palate to facilitate feeding.
- Provides maxillary cross-arch stability after cheiloplasty (lip repair).
- Provides maxillary orthopaedic moulding (before bone grafting).
The maxillary obturator - Construction
- Maxillary Impression- within 2 weeks of birth.
- Modified stock tray.
- The infant was held upright to prevent aspiration.
- Emergency equipment- forced oxygen, suction, standard airway management.
Obturator – Advantages
- Creates a rigid platform on which a baby can press the nipple and extract milk.
- Reduces nasal regurgitation and incidence of choking.
- Shortens time required for feeding.
- It prevents the tongue from entering the defect and interfering with the spontaneous growth of palatal shelves towards the midline.
- It helps correct tongue position for functional development and speech development.
- Reduces the passage of food into the nasopharynx & reduces the incidence of otitis media and nasopharyngeal infections.
Obturator – Disadvantages
- Frequent visits for adjustments and replacements to accommodate growth.
- Repeated construction of new obturators.
- Poor oral hygiene can lead to fungal growth on the palate.
- May be costly.
- Hazards encountered while taking impressions.
- Intraoral placement of other obturators is challenging.
Feeding bottles:
- Mead-Johnson cleft palate nurser
- Haberman feeder
- Type-P teat (Pigeon Co Ltd.)
- Squeezable bottles
- NUK Orthodontic bottles – broader teat, better flow rate
Feeding technique: ESSR technique - Richard (1991)
E = Enlarge nipple hole
Allows formula to reach the back of the infant’s throat.
S = Stimulate the suck reflex by rubbing the teat against the lower lip
Prepares infant for feeding through an enlarged teat.
S = Swallow fluid normally to receive an adequate amount of formula
R = Rest after signal
The infant will exhibit a facial expression that indicates a short break is necessary.
Feeding instructions:

A. Presurgical orthopaedics:
- In bilateral CLP – the premaxilla is severely malpositioned anteriorly or laterally
- Lip surgery at this stage can cause lip dehiscence
- Infant orthopaedics
- To mold alveolus to lessen the severity of cleft
- To enhance surgical repair of lip and nose
- Elastomeric tape
- Intraoral appliances
- Nasoalveolar Molding (NAM)
a. Elastomeric tape
- Hofman (1686)- head cap and premaxillary strap
- Lip taping- across the upper lip
- Allows movement and decreases the width of the cleft
- Applies forces indiscriminately à palatal constriction
b. Latham appliance (1976)
- Dentomaxillary advancement appliance
- Unilateral cleft - approximation of segments
- Bilateral clefts
- expand collapsed lateral cleft segments
- Retract premaxilla
- Maintains palatal width
- Surgically placed with screws
- Requires surgical removal
c. Nasoalveolar molding
- “Pre-surgical Nasoalveolar Moulding (PNAM)” was earlier known as “Pre-surgical orthopaedics”.
- The first PNAM appliance- designed by Grayson et al. (1999).
- Nasoalveolar molding is a nonsurgical method of reshaping gums, lip, and nostrils before CLCP surgery, reducing severity of cleft.
- Primary aim of PNAM is reduction in soft tissue and cartilaginous cleft deformity to facilitate surgical soft tissue repair in optimal conditions under minimum tension to minimise scar formation.
- PNAM should be started as soon as possible after birth.
- Molding of tissue is much easier in the early days of newborns because there is an increased level of maternal estrogen and hyaluronic acid in neonates which increases the elasticity of tissues and hence is favorable for molding.
B. Cheiloplasty
- Lip surgery at 3 months of age
- Improves infant’s appearance
- Performed with primary nasal reconstruction
C. Bone grafting
- When maxillary segments are well-aligned
- Children<2 years – Primary bone grafting
- Children 9-12 years – Secondary bone grafting
D. Primary bone grafting
Indications:
- Elimination of bone deficiency
- Stabilisation of the premaxilla
- Creation of new bone matrix
- Augmentation of alar base
Controversies:
- Grafting may cause growth disturbances in the middle third of the face.
- Vomeropremaxillary suture closure was found to cause inhibition of maxillary growth.
- Most cleft lip and palate centres across the world have abandoned them..
E. Gingivoperioplasty (GPP)
- Utilises osteogenic properties of infants.
- Bridges the bony cleft of the alveolus instead of grafts (boneless bone grafting).
- During lip repair, mucoperiosteal flaps are raised.
- Sealed over alveolar cleft without bone graft.
- Alveolar segments are realigned by presurgical orthopaedics.
F. Palatoplasty
- Closure of the palate – 1 year of age
- To facilitate the acquisition of normal speech
- May improve hearing and swallowing
G. Dental care
- Infant oral health care
- “Age one” dental visit (AAPD)
- Oral examination
- Soft/hard tissue anomalies Anticipatory guidance
- Prevention of oral disease
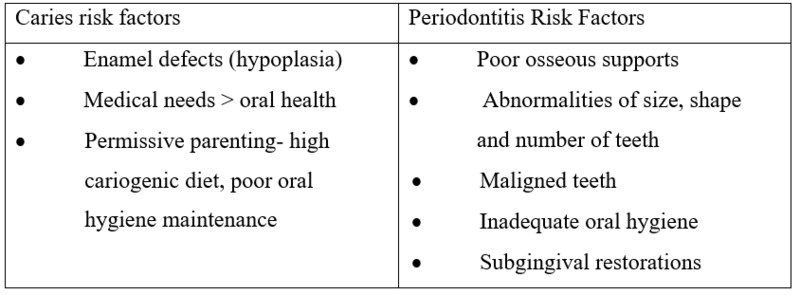
- Oral health risk factors with CLP
2. Stage II: Primary dentition stage: 18 months to 5 years
- Establishing and maintaining oral health.
- Increased frequency of periodic examinations (3-4 months).
- Extensive unilateral/bilateral clefts- surgical closure postponed beyond 12 months of age.
- Maxillary prosthetic appliances.
3. Stage III: Late primary or early mixed dentition 6-11 years of age
- Correction of Ectopically erupting permanent central and lateral incisors
- Posterior crossbite
- Correction of developing traumatic occlusion
- Maxillary expansion to correct posterior segment collapse
- Secondary Alveolar Cleft Bone Graft: It provides
- Bony support for teeth adjacent to the cleft
- Maxillary arch continuity
- Closure of oronasal fistula
- Supports the alar base of the nose
- Done before orthodontic tooth alignment
- 2 months after bone graft- orthodontic movement
- Periodontal support to erupting teeth
- Stabilisation of premaxilla (in bilateral cleft cases)
- 90% success rate
- Morbidities include pain in the donor site, dehiscence of mucosal flaps, and partial or complete loss of grafted bone.
4. Stage IV: Permanent dentition stage 12-18 years
- Orthodontic-surgical management: Correction of retrusive maxilla LeFort I maxillary advancement.
- Cosmetic surgery: Restore projection, symmetry, refinement and airflow to the nose, Cartilaginous nasal tip asymmetries correction.
A paediatric dentist must consider the impact cleft lip and palate may have on the physical, mental, and emotional well-being of the child, and work closely with other members of the health care team to provide the most comprehensive care possible.
Disclaimer- The views and opinions expressed in this article are those of the author and do not necessarily reflect the official policy or position of M3 India.
About the author of this article: Dr Neha Kalantri is a practising dentist from Nashik.
-
Exclusive Write-ups & Webinars by KOLs
-
Daily Quiz by specialty
-
Paid Market Research Surveys
-
Case discussions, News & Journals' summaries